Adhesive capsulitis, commonly known as frozen shoulder, is a painful and debilitating condition that causes progressive stiffness and limited mobility in the shoulder joint. If you’re dealing with increasing shoulder pain and difficulty raising your arm, reaching behind your back, or performing daily tasks, you may be experiencing frozen shoulder. This condition affects millions worldwide, particularly adults aged 40-65, and while it can resolve over time, early intervention often speeds recovery and improves quality of life.
In this comprehensive guide, we’ll cover everything you need to know about adhesive capsulitis (frozen shoulder) — including its causes, stages, key symptoms, diagnosis, effective treatment options, recovery timeline, and practical tips for managing it in 2026.
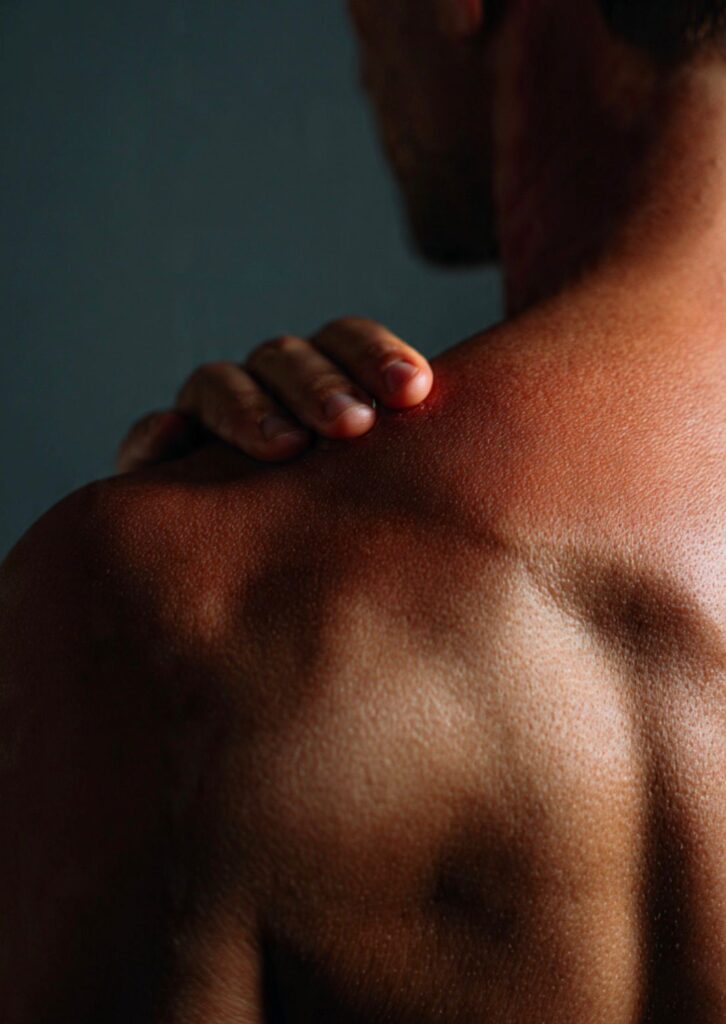
What Is Adhesive Capsulitis (Frozen Shoulder)?
Adhesive capsulitis occurs when the connective tissue capsule surrounding the shoulder joint becomes inflamed, thickened, and tight. This leads to the formation of scar tissue (adhesions) and reduced synovial fluid, restricting joint movement. The result? Severe pain and a “frozen” shoulder that feels stuck.
Unlike injuries from trauma, frozen shoulder often develops gradually without a clear trigger. It’s more common in one shoulder, though it can affect both over time. Women are at higher risk, especially during perimenopause or with hormonal changes.
Common Causes and Risk Factors of Frozen Shoulder
The exact cause of adhesive capsulitis remains unclear, but inflammation triggers the capsule to tighten. Known risk factors include:
- Age (most common between 40-65 years)
- Gender (women affected more than men)
- Diabetes (significantly higher risk, especially poorly controlled)
- Thyroid disorders (hypo- or hyperthyroidism)
- Previous shoulder injury, surgery, or immobilization (e.g., after rotator cuff tear or fracture)
- Other conditions like heart disease, Parkinson’s, or stroke
- Hormonal changes (e.g., menopause)
Early recognition of these factors can help prevent prolonged symptoms.
The Three Classic Stages of Frozen Shoulder
Frozen shoulder progresses through three overlapping stages, each lasting months if untreated:
- Freezing Stage (Painful Phase – 2-9 months): Pain dominates, especially at night or with movement. Range of motion begins to decrease gradually.
- Frozen Stage (Stiff Phase – 4-12 months): Pain may lessen slightly, but stiffness peaks. Daily activities like dressing, driving, or sleeping become challenging.
- Thawing Stage (Recovery Phase – 5-24 months or longer): Pain subsides, and mobility slowly returns. Full or near-full recovery is possible, though some experience lingering mild stiffness.
Total duration often spans 1-3 years, but proactive treatment can shorten this significantly.
Key Symptoms of Adhesive Capsulitis
Look for these hallmark signs:
- Dull, aching shoulder pain (worse at night or with attempted motion)
- Progressive stiffness and limited range of motion (both active and passive)
- Difficulty raising the arm overhead, reaching behind the back, or across the body
- Pain that interferes with sleep and daily tasks
- Usually affects one shoulder (bilateral in rare cases)
If symptoms persist beyond a few weeks without improvement, consult a healthcare provider promptly.
How Is Frozen Shoulder Diagnosed?
Diagnosis relies on:
- Medical history and symptom description
- Physical exam (assessing active/passive range of motion)
- Ruling out other conditions (e.g., rotator cuff tear, arthritis) via imaging like X-ray, ultrasound, or MRI if needed
No single test confirms adhesive capsulitis, but restricted motion in multiple planes is diagnostic.
Effective Treatment Options for Frozen Shoulder in 2026
Most cases respond well to non-surgical approaches. Treatment focuses on pain relief, restoring motion, and preventing further stiffness.
- Physical Therapy — Cornerstone of management. Includes gentle stretching, range-of-motion exercises, manual therapy, and strengthening. Early structured PT accelerates recovery.
- Pain Management — Over-the-counter NSAIDs (e.g., ibuprofen) for inflammation. Heat/cold therapy for comfort.
- Corticosteroid Injections — Intra-articular steroids provide strong short-term pain relief (especially in freezing stage) and improve function when combined with PT.
- Hydrodilatation (Distension) — Injecting saline to stretch the capsule; often ultrasound-guided for precision.
- Other Interventions — Emerging options like shockwave therapy, suprascapular nerve blocks, or platelet-rich plasma (PRP) show promise for refractory cases.
- Surgery — Rare (e.g., manipulation under anesthesia or arthroscopic release) for persistent severe cases after conservative failure.
Always tailor treatment to your stage and overall health — consult an orthopedist or physical therapist.
Recovery Timeline and Prognosis
With consistent treatment:
- Many see noticeable improvement in 3-6 months
- Full recovery often occurs within 1-2 years
- Most regain near-normal function, though mild residual stiffness can linger in some
Patience is key, but avoiding immobility worsens outcomes. Regular gentle movement prevents “re-freezing.”
Prevention Tips and Home Management Strategies
- Stay active after shoulder injuries or surgery with early motion
- Manage diabetes and thyroid conditions effectively
- Perform daily gentle shoulder stretches if at risk
- Use proper posture and avoid prolonged arm immobilization
When to See a Doctor for Frozen Shoulder
Seek medical advice if:
- Shoulder pain and stiffness last more than a few weeks
- Night pain disrupts sleep
- Daily activities become impossible
- Symptoms follow injury or surgery
Early intervention often leads to faster thawing and less frustration.
Adhesive capsulitis (frozen shoulder) is challenging, but highly manageable with the right approach. By understanding its stages, addressing risk factors, and committing to evidence-based treatments like physical therapy and targeted injections, most people regain shoulder function and return to pain-free living.
If you’re experiencing these symptoms, don’t wait — reach out to a healthcare professional today for personalized guidance. Recovery is possible, and starting early makes all the difference.